Patellar dislocation, kneecap dislocation, dislocation of the kneecap, patellar dysplasia, cartilage damage behind the kneecap, cartilage flake, articular mouse, rupture of the medial retinaculum
In the typical dislocation of the kneecap, the kneecap jumps out of the intended slideway. This often leads to ligament, cartilage and bone injuries.
Also read our topic Kneecap jumped out
Women are more often affected by a dislocation of the kneecap than men
The first dislocation event usually occurs before the age of 20.

$config[ads_text1] not found
Who am I?
My name is dr. Nicolas Gumpert. I am a specialist in orthopedics and the founder of .
Various television programs and print media report regularly about my work. On HR television you can see me every 6 weeks live on "Hallo Hessen".
But now enough is indicated ;-)
The knee joint is one of the joints with the greatest stress.
Therefore, the treatment of the knee joint (e.g. meniscus tear, cartilage damage, cruciate ligament damage, runner's knee, etc.) requires a lot of experience.
I treat a wide variety of knee diseases in a conservative way.
The aim of any treatment is treatment without surgery.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You can find me in:
Directly to the online appointment arrangement
Unfortunately, it is currently only possible to make an appointment with private health insurers. I hope for your understanding!
Further information about myself can be found at Dr. Nicolas Gumpert
$config[ads_text2] not found
In most cases it is an unfavorable combination of components that promote dislocation.
From an anatomical point of view, a knock-kneed leg, an incorrectly placed kneecap (patellar dysplasia, so-called hunter's hat patella) and an insertion of the patellar tendon that is too far out are risk factors.
On the part of the ligamentous apparatus, a loose ligamentous apparatus applies (ligament laxity = hypermobility of the patella) and a raised patella (patella alta) as unfavorable.
Muscularly, there is an imbalance of the outer and inner anterior Thigh muscles dislocation-promoting.
The more risk factors that come together, the higher the likelihood of a kneecap dislocation.
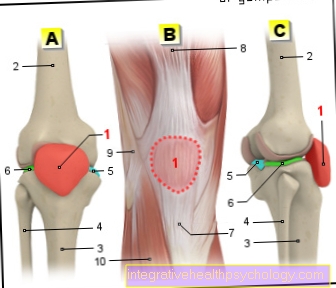
You can find an overview of all Dr-Gumpert images at: medical illustrations
$config[ads_text3] not foundThe kneecap stability is divided into three degrees of instability of the kneecap:
$config[ads_text2] not found
1. Patellar lateralization (The kneecap slides too far outside (laterally) in the kneecap sliding bearing
2. Subluxation of the kneecap (the kneecap almost dislocates)
3. Dislocation of the patella (complete dislocation of the Kneecap)
The first kneecap dislocation with an accident event is medically called traumatic dislocation of the kneecap designated. Renewed dislocation events are called chronic recurrent (post-traumatic) patellar dislocation.
A kneecap dislocation that occurs without a real accident event is called habitual patellar luxation designated. The kneecap jumps out of its plain bearing and back in again without any major discomfort. This instability is particularly evident in the first 45 ° of flexion.
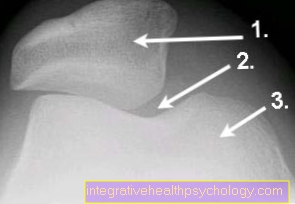

Patellar luxation can be diagnosed by looking at it alone. In almost all cases, the kneecap jumps outward beyond the intended slideway. It is visible there, the patella sliding bearing is empty.
In most cases, what is known as self-repositioning occurs. This means that the kneecap jumps back into its slideway with slight movements.
In these cases a detailed medical history is necessary.
When the kneecap dislocates, the inner ligament and holding apparatus of the kneecap (medial retinaculum) tears. As the kneecap moves out of the slideway, further damage to the kneecap and the thigh bone often occurs.
The result of the traumatic dislocation of the kneecap is an effusion of the knee joint (joint effusion) and significant pressure pain under the inner kneecap facet (tear (rupture) of the medial retinaculum).
The sudden sagging of the knee joint during the dislocation process (giving way) speaks for a traumatic patellar dislocation.
Find out more about: Acute knee pain - that may be behind it
The symptoms of a kneecap dislocation (kneecap dislocation) are mostly like this typicalthat she is a trained doctor Eye diagnosis enable.
However, it must be remembered that very often the kneecap, especially if it slipped out of position for the first time in an accident, spontaneously slips back into its sliding bearing (Self-repositioning).
It is therefore important that if a kneecap dislocation is suspected, a thorough medical history (systematic medical survey) is collected, even if appropriate Symptoms currently no longer exist.

In most cases tears in the case of a dislocation of the kneecap inner band and holding apparatuswhich is why they are usually outwardly slips out over the slideway provided for it.
Various indications suggest a dislocation of the kneecap:
Through the pain and the Joint effusion is the agility in the knee joint highly limited or no longer possible at all.
$config[ads_text1] not found
Apart from these acute symptoms, a dislocation of the kneecap can be diverse Concomitants and complications come:
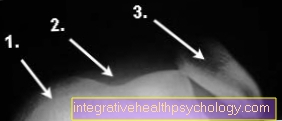
If the kneecap is still dislocated, the diagnosis can be made by looking at it alone.
In addition, the knee joint effusion and the giving way are groundbreaking for diagnosis.
The so-called apprehension test is carried out as a clinical examination. An attempt is made in the relaxed state to push the kneecap over the outer plain bearing. The test is positive if an involuntary defensive movement is performed or the kneecap can be dislocated.
An X-ray image of the knee joint is carried out on the basis of diagnostic equipment.
In addition, a special image of the kneecap is made in three positions (patellar filet at 30 °, 60 ° and 90 ° flexion of the knee joint). This image can be used to assess patellar dysplasia (misalignment of the patella), osteoarthritis behind the kneecap (retropatellar arthrosis) and osteoarthritis of the bone (cartilage flake).
If there is an urgent suspicion of cartilage shearing off the posterior surface of the kneecap or the outer thigh roller (femoral condyle), a magnetic resonance imaging of the knee joint (MRI knee) should be performed in order to determine the extent of the damage.
In addition to the cartilage damage, the ligament injury can also be assessed in magnetic resonance imaging of the knee joint, especially the medial retinaculum of the kneecap, which often tears completely outward in the event of a kneecap dislocation.

In most cases, a kneecap dislocation does not require any treatment, as it usually springs back into its sliding bearing by itself (Self-repositioning), especially when the knee joint is brought into an extended position.
If this does not happen, however, it is extremely important, a kneecap dislocation quickly and adequately to treat possible To avoid consequential damage.
The aim is to permanently bring the kneecap back into its plain bearing, since every new dislocation the Increased likelihood of cartilage damage.
First of all, the kneecap needs to be brought back into its correct position as soon as possible. This Reduction can either be through a doctor or one experienced sports trainer respectively. Here it is important that Slowly straighten your knees and the Kneecap with it firmly in handso that there are no sudden unwanted movements.
If the reduction is successful, it makes itself felt for the patient Immediate improvement in pain noticeable.
in the connection if possible a X-ray or one Computed tomography (CT) to confirm the correct position of the kneecap.
Depending on how severe the damage is, you can choose between various treatment options choose.
The Treatment of a dislocation of the kneecap usually begins with a conservative attempt before resorting to surgical measures, which in 50% of cases can already lead to permanent success.
Only if the therapy is unsuccessful or if there is a renewed dislocation, surgical therapy is used.
The conservative therapeutic approach here consists of physical therapy and the Application of bandages, Orthotics, Plaster sleeves or Tapes.
With the help of these measures, an attempt should first be made to restrain and strengthen the kneecap-guiding muscles (especially the quadriceps muscle). The application of tapes - preferably Kinesio tapes - pursues the goal of bringing the kneecap into the correct position or into its guide rail in order to enable smooth movement in the knee joint and to prevent it from slipping (again). It therefore serves to easily fix the kneecap in its correct position.
In addition, the application of a kinesio tape can also reduce pain and inflammation, provided that one of the two has previously existed in the context of the kneecap dislocation or the existing kneecap malalignment.
Correct treatment following a dislocation of the kneecap is of great importance, otherwise consequential damage such as a arthrosis can train. There is also a increased risk of dislocating the kneecap again and this also increases the likelihood of complications.
One usually tries that first Treatment conservatively, so without a surgeryto perform.
However, under certain circumstances it may be necessary to have surgery.
Factors in favor of an operation are:
Of course it is always the same Patient's request decisive for whether it ultimately comes to the operation or not.
Which of the available operations is preferred in an individual case depends on:
The target of all procedures it is that restore normal anatomy in the knee joint.
As part of the operation it is important on the one hand Cartilage damage to remedy and on the other hand, any existing ones free pieces of bone or cartilage from the joint to remove. These distances can normally already be carried out during the diagnosis Artoscopy from the knee (Arthroscopy) respectively.
Usually one uses it then primary the Soft tissue surgeryif these lead to a cure with a high probability and only in more extreme cases will be on bony correction methods (which can also only be used after growth has been completed).
Different operative interventions can be distinguished:
Both methods can be used with the so-called "Lateral release" be combined. This is characterized by the fact that the Band structures on the outside the kneecap severed be, whereby the The tendency of the kneecap to jump outwards is no longer so strong given is.
There are still, however many other ways to surgically treat a dislocation of the kneecap.
in the Following the operation however, the treatment phase is not yet over. Depending on which procedure was chosen, the patient has to do this for a certain period of time Relieve the knee joint and then regularly physiotherapy operate to too a correct position of the kneecap in the long term to guarantee.
The follow-up treatment after a reconstruction operation for a dislocation of the kneecap amounts to 4 phases:
Any dislocation of the kneecap is a serious injury to the knee joint that is often associated with permanent damage.
This is why optimal follow-up treatment for often young patients is particularly important.
Even with ideal follow-up treatment of a patellar dislocation, damage to the cartilage sliding surface of the kneecap and thigh must be expected in the medium and long term.
The greatest goal must be to keep this damage as low as possible in order to ensure permanent pain-free function of the knee joint.