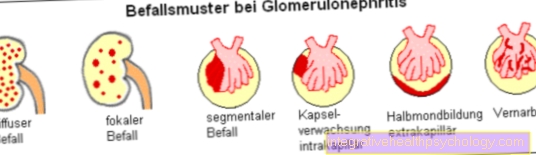
The therapy, the chances of success of the therapy and the forecast depend largely on the form of glomerulonephritis. In most cases there is one Immunosuppression displayed.
Also read:
You are on a "Forms of Glomerulonephritis" subpage. General information on the subject can be found on our Glomerulonephritis page. Gomerulonephritis often leads to another clinical picture, which is called nephrotic syndrome.
Also read: Nephrotic Syndrome
A basic distinction is made between the following forms:
$config[ads_text1] not found
Minimal-Change Glomerulonephritis
In this variant, the so-called Foot cells disturbed. As a result, the negative charge of the filter is lost and proteins are filtered. Besides the Proteinuria (Loss of proteins via the kidneys) or Albuminuria (Loss of proteins via the albumin) occur Weight gain and Water retention (edema) as well as a nephrotic syndrome on.
Typically, children get sick between the ages of 2 and 6 years. It is believed that certain immune cells in the blood (T cells) produce and release a substance that damages the foot cells.
The root cause is still unknown. In rare cases, however, a connection with certain drugs, some cancers or after transplantation with stem cells has been proven.
The therapy consists essentially of the gift of Immunosuppressants and symptomatic treatment such as the flushing out of edema with diuretic drugs.
In the Post-streptococcal glomerulonephritis / acute post-infectious glomerulonephritis a few weeks after an infection with certain pathogens (e.g. ß-haemolytic streptococci of group A), the person affected develops a slight fever and pain in the joints and the Kidney region.
The decreased amount of urine (oligoury) is red-brown (as a sign of blood filtration) and water retention (edema) occurs. High blood pressure is also typical. Antigen-antibody complexes are deposited, which lead to the destruction of the filter.
In the age of antibiotic therapy, the Forecast quite good. In Western Europe, the disease heals in more than 90% of children with an adequate therapy start and regimen; in adults, the rate is around 50%.
If it is a different pathogen, the prognosis is worse. Non-streptococcal conditions can, for. B. inflammation of the Lining of the heart (endocarditis) or one Blood poisoning (sepsis) be the cause of post-infectious glomerulonephritis.
Mesangial cells are connective tissue cells in the small blood vessels in the kidney filter.
IgA (immunoglobulin A) is one of certain Blood cells (plasma cells) antibody produced. This shape is also known as IgA nephropathy or Berger's nephritis. It is the most common form of Glomerulonephritis, which mainly affects young men and which can have very different courses.
The most common symptoms are Blood in the urine (Hematuria),
$config[ads_text2] not found
$config[ads_text3] not foundFlank pain and high blood pressurethat needs to be treated consistently, as well as proteinuria. The hemuria or proteinuria can be so minor that in the absence of other symptoms it is often discovered only by chance. The history of its origins (pathogenesis) is still unclear.
It is noticeable, however, that it occurs more frequently in families, so that one genetic predisposition (genetic predisposition) is suspected. There is no therapy against the cause. A combination seems promising if you start in time Corticosteroids and Immunosuppressants to be.
About half of those affected show a chronic form, which is not infrequently a chronic renal failure ends.
A pathological hardening of the organ (sclerosis) and an accumulation of a glass-like, transparent substance called hyaline (hyalinosis) in individual glomerular sections are evident in the microscopic preparation.
The Emergence this form is not clarified, however, is more common at HIV-infected people or heroin users.
More than 30% of the cases are chronic up to Renal failure. Even after one Kidney transplant there is a high rate of recurrence.
There is no systematic therapy. Therapy with suppression of the immune system is sometimes successful.
The membranous glomerulonephritis often appears for no apparent cause. However, it sometimes occurs with certain medical conditions such as:
Immune complexes are deposited on the outside of the basement membrane. A third heals spontaneously, another third shows chronic protein loss via the urine and in a third of the patients the disease progresses to renal insufficiency.
Membranous glomerulonephritis is the most common cause of nephrotic syndrome.
$config[ads_text4] not found
Also membrane proliferative glomerulonephritis is rather rare and of unknown cause.
It is often associated with a hepatitis or malignant lymph node degeneration found.
At the beginning, a nephrotic syndrome often appears with progressive symptoms up to Renal failure. There is currently no effective therapy available. After 5 years, around 50% of those affected have to undergo a machine blood purification process (dialysis) take advantage of.
In the necrotizing intra- / extracapillary proliferative glomerulonephritis the focus is on the rapidly progressing course over a few weeks and months.
The Symptoms include:
This form can occur as a severe course of glomerulonephritis with immune complex formation (e.g. post-streptococci GN) or in the variant with antibody formation against the basement membrane. But it can also go hand in hand with no immune complex deposition. It is characterized by pathological cell death (necrosis).
The tissue examination also reveals crescent-shaped proliferation. Linear deposits of antibodies of the IgG type along the basement membrane are found in histological preparations of the form with antibody formation against this basement membrane (e.g. Goodpasture Syndrome).
The Therapy success depends on Start treatment from. The focus is on immunosuppression and the administration of corticosteroids, supplemented by a mechanical exchange of the blood plasma (plasmapheresis).
If therapy is initiated quickly and when the creatinine level is below 6 mg / dl, the prognosis is favorable.
In most cases, however, a partial loss of function remains. From a creatinine level of 6 mg / dl, the prognosis is poorer and often ends in the need for dialysis.
<- Back to the main topic Glomerulonephritis